Critical Point of Health Care
The mortality rate in Covid-19 cases illustrates the ability of the health care system to treat Covid-19 patients, which is affected by the availability of the number of beds, personnel, medical equipment and medicines.

The government through the Covid-19 task force on 20 December announced that the number of deaths from Covid-19 had reached a new record.
(That day) as many as 221 deaths from Covid-19 cases were reported, with the total number of Covid-19 deaths reaching 19,880. The increase in the Covid-19 mortality rate is a sign of a critical situation in the health care system in Indonesia, particularly in managing Covid-19 patients.
Also read: “Long Covid”, the Covid-19 Aftermath
The mortality rate in Covid-19 cases illustrates the ability of the health care system to treat Covid-19 patients, which is affected by the availability of the number of beds, personnel, medical equipment, medicines and other supporting facilities.
Causal factor
The mortality rate increase reflects the strong pressure on the health care system in Indonesia, which is also marked by the high occupancy of hospital beds in almost all provinces in Indonesia, especially in Java. Data in several regencies and cities in Central and East Java shows that the level of occupancy of beds in hospitals has reached 90 percent, much higher than the WHO standard, which is a maximum of 70 percent.
This has resulted in an accumulation of the number of Covid-19 patients who need treatment and delays in handling, which have led in the worsening of the patient\'s condition and leading to death. The contribution of health care capacity is shown by the relatively low case fatality rate (CFR) in Jakarta, which stood at 1.9 percent compared to CFR in Central Java, which reached 4 percent and East Java, which reached 6.9 percent. With a health care capacity that is relatively larger than other provinces, patients with moderate and severe symptoms can be treated more quickly and reduce the risk of death, even though Jakarta has the largest number of confirmed cases in Indonesia.
Also read: Vaccines as Public Goods
Another problem related to Covid-19 health care in Indonesia is the quality of service indicated by the national Covid-19 CFR, which is higher than the global average. Quality health care is able to minimize the mortality rate among Covid-19 patients. Although the clinical management of Covid-19 cases is still not definitive in the absence of a specific antiviral for Covid-19, patients with moderate, severe and critical symptoms must receive intensive therapy to prevent death.
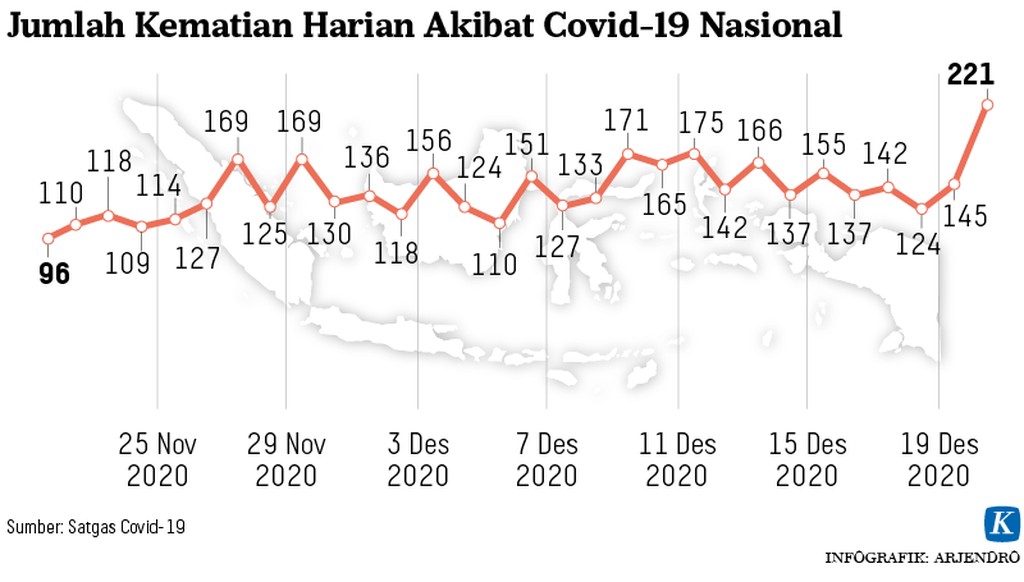
National Number of Daily Deaths Due to Covid-19. Source: Covid-19 Task Force
The provision of latest drugs, such as the antiviral Remdesivir, the anti-inflammatory Toclizumab, experimental monoclonal antibodies or conventional plasma therapy should be undertaken. In addition, the availability of intensive care rooms and ventilators is essential for patients in critical condition. Until now, this therapeutic modality has not been evenly distributed in Indonesia, even in Java at the regency and city levels.
Also read: Optimism in Welcoming Vaccines
This has caused patients, who experienced worsening conditions from moderate to severe and from severe to critical, do not or are too late to get an ideal therapy because of the absence of latest medicines, ventilators and intensive rooms. The addition of ventilators and intensive rooms recently has not been able to cover the existing shortcomings, given that the distribution problem of the quantity and quality of the health care is a chronic problem that has lasted for decades in Indonesia.
Impact
The pressure due to the Covid-19 pandemic will have negative impacts on the sustainability of Indonesia\'s health care system. The high mortality rate of Covid-19 cases is a clear direct indicator. Another impact is the high rate of Covid-19 transmission among health workers in Indonesia. The excessive workload leads to burnout among the health workers, reduces self-awareness in protecting against Covid-19 infection and also reduces immunity. The transmission among the health workers makes health facilities a potential source of infection.
Health facilities that become source of transmission will limit and even close services. This disrupts the continuity of health services for other diseases, such as diabetes and cancer. The delay in diagnosis and treatment of these diseases will result in an increase in the complication rate and death, which is commonly referred to as excess mortality or silent pandemic. The phenomenon of excess mortality has been proven to take place in developed countries although it is still difficult to demonstrate in Indonesia due to the absence of data. Sporadically, a decrease in access to maternal health services, such as delivery with difficulty, as well as treatment of chronic infectious diseases, such as tuberculosis and HIV/AIDS, has been widely reported in Indonesia and has the potential to increase mortality rates.
Also read: What Needs to be Considered From the New Vaccine
The high rate of infection among health workers also results in high mortality rates among the health workers in Indonesia. The reduction in the number of doctors will further reduce the capacity of health care in Indonesia, which is still inadequate.
Doctors are trained professionals who require a minimum education process of six years, or even more, for specialists and sub-specialists. The number of doctors produced, especially specialists and subspecialists, is also very limited, considering that not all medical schools in Indonesia have the authority to run a specialist and sub-specialist medical education. The lack of health personnel with very specific expertise will further widen the gap in the quality of health care in Indonesia. Patients with high socioeconomic abilities take medication abroad to get quality services, while low-income people cannot afford health services. There are two losses, both in terms of health, with the inability to achieve quality public health status as well as in term of economy with the wasting of foreign exchange for medical purposes abroad.
Also read: Acceptance, the Key to Vaccination

FILE - In this Dec. 7, 2020, file photo, released by Indonesian Presidential Palace, workers spray disinfectant on boxes containing experimental coronavirus vaccines made by Chinese company Sinovac arriving at a facility of state-owned pharmaceutical company Bio Farma, in Bandung, West Java, Indonesia. With rich countries snapping up supplies of COVID-19 vaccines, some parts of the world may have to rely on Chinese-developed shots to conquer the outbreak. The question: Will they work?
Mitigation measures
Mitigation efforts to reduce pressure on the health care system in Indonesia must be carried out immediately. This pressure can be reduced if the increase in the number of cases can be curbed and the service capacity can be increased. However, it must be remembered that in a pandemic situation, the increase in the number of cases is exponential and the increase in the capacity of health care is linear. Thus, efforts are needed to reduce the growth of cases drastically.
There is no magic formula in this matter other than implementing the “3M” health protocol (washing hands, wearing masks and keeping physical distance) coupled with massive and consistent restrictions on the mobility of society. Without limitation on mobility, 3M implementation, especially maintaining physical distance, is ineffective because the existing public spaces are not designed to accommodate public activities while maintaining distance.
The next step is the implementation of “3T” (testing, tracing, to follow-up) to separate confirmed cases as sources of transmission from the healthy population. Increasing the coverage of standardized testing, intensive tracing of close contacts and effective patient isolation should be conducted more seriously.
Without more serious efforts to deal with the pressure on the health care system, the mortality rate among the Covid-19 patients will continue to increase.
Increasing the capacity of health care remains crucial to reduce mortality. Increasing the number of beds, the latest medicines and equipment, such as ventilators that are evenly distributed across regencies and cities is the key. The flow of medical treatment should be set by prioritizing patients with moderate and severe symptoms for hospitalization. The availability of non-hospital health care facilities needs to be assured to make the treatment effective for asymptomatic patients and those with mild symptoms.
To ensure a health care standard, hospital categorization and zoning can be applied. This categorization limits the authority of the hospital to treat patients according to their capabilities so that patients actually get optimal care according to the severity of the disease. Hospital conversion from a public hospital into a Covid-19 only hospital can be done to increase the effectiveness of treatment. The existence of a specialized hospital makes it easy to mobilize and distribute the necessary resources as well as the possibility of cross-infection for the general patient.

Joko Mulyanto
Without more serious efforts to deal with the pressure on the health care system, the mortality rate among the Covid-19 patients will continue to increase and the collapse of the Indonesian health care system is only about time.
Joko Mulyanto, Lecturer and Researcher of Health Services, Department of Public Health and Community Medicine, School of Medicine, Jenderal Soedirman University.
This article was translated by Kurniawan Siswoko.