Watching out for Long Covid
Many mistakes were made previously for during the phase of acute Covid-19 infection. There is no reason to fail again in responding to long Covid. There is no more time to waste.

It is feared that the two-year pandemic could give rise to a hidden crisis: long Covid. Also called post-Covid syndrome (PCS), this crisis even threatens many developed countries with fairly high rates of vaccination like the United States and the United Kingdom.
The threat could be more serious with the spread of the new Omicron strain and the emergence of the latest variant, provisionally named the IHU variant (after the research institute that helped identified it, Instituts hospitalo-universitaires) in Marseille, France. The new strain, B.1.640.2, contains 46 mutations, more than the mutations in the Omicron variant, and is feared to be more infectious and more resistant to vaccines.
Long Covid presents a group of symptoms (a syndrome) in certain parts of the body around three months after an acute Covid-19 infection. Three important symptoms frequently arise: shortness of breath, fatigue and brain fog.
Also read:
> Riding out the Omicron storm
Three out of five (60 percent) long Covid patients in the UK have said the syndrome made it “rather difficult” to engage in daily activities, while one out of five (20 percent) maintained it was “very difficult” to conduct activities, even a part-time desk job.
Since the outset of the pandemic, many reports have indeed mentioned the emergence of patients experiencing symptoms related to the nervous system and brain function. The neurological symptoms usually appear during or after an infection. Besides fatigue and brain fog, the disorders can vary, including convulsions and strokes.
Shrouded in mystery
Many cases are still shrouded in mystery. Brain fog is in itself, according to an article published to the Harvard Health website on 8 March 2021, not a medical term, but rather a term people use to explain a condition in which their thought processes are disrupted or they feel their brain is weak and dull. In brief, they find it difficult to concentrate.
In “normal” times pre-Covid-19, this condition can last several hours, for instance, as a result of jet lag, flu or a side effect of consuming certain drugs. However, there is concern that brain fog persists in long Covid patients.
A study conducted by Jan Wenzel and his team at the University of Lübeck, Germany, which was published in the Nature Neuroscience journal (21/10/2021) and cited by Forbes (8/12/2021), explains that some Covid-19 patients showed structural damage in the capillaries that supply blood to the brain.
Supriyanto
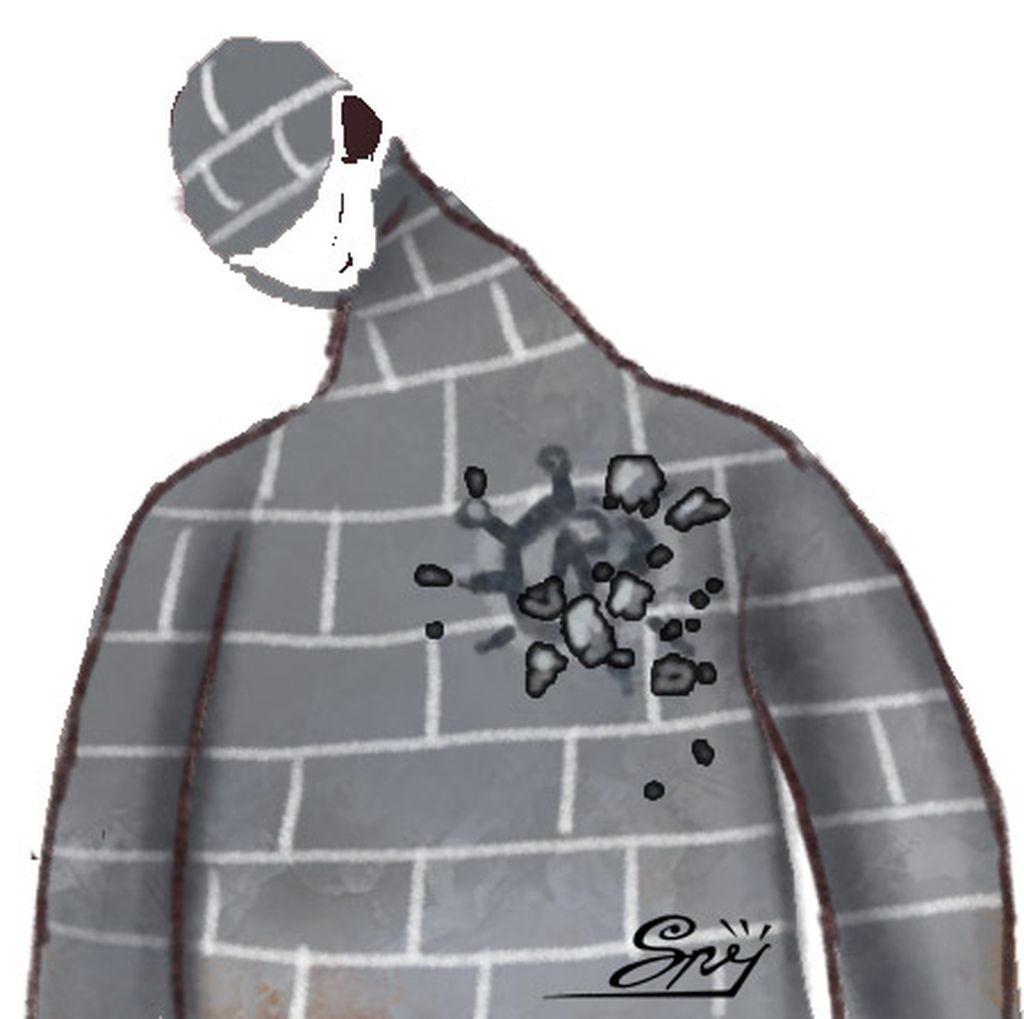
What might happen is that the endothelium cells that form the capillary walls are destroyed by the protease produced by SARS-CoV-2, the virus that causes Covid-19. A protease is an enzyme that speeds up the breakdown of proteins into amino acids, like the protein breakdown that occurs in the digestive tract.
A description is necessary here. The walls of all blood vessels, from major arteries to capillaries, are made of several layers. Imagine the walls of our houses made of brick, cement, sand and paint on both sides. The difference is that while the walls of a house are “dead”, the walls of a blood vessel, like all tissues in our bodies, are alive and continue to regenerate sustainably.
The thinnest layer of tissue in the innermost wall of the blood vessel is called the endothelium, a lining that is in direct contact with the blood cells that pass through the vessels. This lining filters everything that enters and leaves the bloodstream. Endothelium cells also have an important role in forming networks of blood vessels, emitting signals to help build blood vessel walls.
If the endothelium cells die, they will cause string vessels, a condition that occurs when certain parts of a capillary experience a vacuum, so the capillaries fail in their function to distribute blood. If the string vessels become widespread, brain tissues suffer damage to result in brain pathology.
Also read:
> “Long Covid”, the Covid-19 Aftermath
> Beware of Third Wave of Pandemic
A damaged endothelium lining may resemble a pipe that carries water from a pump to residential houses that becomes clogged. It is thus logical that damage to the capillary structure supplying the brain with blood causes a brain functional disorder. According to Jan Wenzel and his peers, although direct infection of the brain is still debated, examining the SARS-CoV-2 genome present in the brain and cerebrospinal fluid in several patients showed that the virus can gain access to the brain.
In fact, there is a view that not all symptoms resembling those of long Covid are caused by SARS-CoV-2. Long before the coronavirus appeared, many healthy people had shown similar symptoms. Their cause cannot yet be explained medically. Among the classic examples of such mysterious conditions is chronic fatigue syndrome, which generally seems to follow a viral or bacterial infection.
Before Covid-19, several types of frequently occurring symptoms, such as chronic migraines, also plagued many people without any apparent cause. Nonetheless, the latest data indicate that long Covid is the dominant cause behind the various prevalent symptoms.
Drugs for the first two disorders may finally be invented. The US has already spent around US$1.15 billion on research. But at present, patients still have to endure several months of rehabilitation to get back to normal.
The 1890s saw the biggest pandemic in history known as the Russian flu that killed around 1 million people. The name is today considered a mistake. It was most likely not influenza, but rather an ancestral type of the coronavirus. At that time, very few people had immunity against it, so the disease became lethal. It is also believed that when the pandemic had ended, it left a wave of new disease that attacked the nervous system.
Who knows that it was similar to long Covid in the present? The same kind of syndrome emerged after the next pandemic, the Spanish flu in 1918. So now, the same thing is happening with Covid-19. The post-infection called long Covid is appearing in countries where acute cases are declining. The condition’s formal definition indeed remains “fluid” as knowledge about it continues to grow.
New hopes
We have no idea yet of the incidence rate of long Covid in Indonesia. But in the UK, the terrible incidence rate is already apparent. According to The Economist (1/5/2021), 500,000 British people have suffered more than six months from long Covid. Their chance for complete recovery seems small, and the majority of cases were present in people of productive age. It is estimated that around 15 percent of the UK population has been infected with long Covid.
If the same figures are applied to Covid-19 cases in the world, which totaled around 1.2 billion people as of May 2021, it can be estimated that over 80 million people have had long Covid.
Also read:
> Third Wave of Pandemic, Threat or Illusion?
> Preventing the Resurgence of Covid-19 Cases
Yet fortunately new hope has now emerged. better vaccines and treatments for Covid-19 as well as several other diseases are expected by the end of 2022. Although millions of people infected during the pandemic remain sick, struggling with difficulties as a result of a combination of around 200 symptoms that manifest as long Covid, the middle of 2022 is expected to bring bright news for most long Covid patients.
This is because many studies on long Covid research that were started in 2021 have begun to show promising results, as demonstrated by the efforts of several developed countries. According to an article from The Economist health correspondent Slavea Chankova published on 8 Nov. 2021, the US National Institutes of Health, for example, has disbursed more than $1 billion to investigate the various causes of and treatments for this condition, while the UK is conducting more than 15 studies involving thousands of long Covid patients.
Major findings are expected in at least three areas.
The first is a biological map of the most severe symptoms of long Covid, such as shortness of breath and brain fog. Several studies, for instance, are trying to discover what changes are affecting the volume and structure of the brain.
Understanding whether the long Covid symptoms are caused by particular tissue damage to blood vessels, the nervous system or the organs, will help contribute to the development of a variety of appropriate treatment methods.
The second area of research focuses on diagnostic tests and scans to track the impacts of long Covid on certain organs in the body. A study in the UK, for example, introduces xenon, a nontoxic gas, into a patient’s body for observing in scans of the gas as it flows through the body. Its results could indicate whether the breathing difficulty was caused by damage to the lungs or the blood vessel tissue.
Another study is trying to find out what happens to cytokines, molecules that have the potential to effect a hyperactive immune response, which has so far been suspected of causing incidences of long Covid. Many such studies will be useful in tracking how long Covid symptoms respond to different therapies.
Our health system and health care companies should prepare assistance for long Covid patients. Proper rehabilitation can prevent permanent damage to personal health and finances.
The third area concerns holding large-scale clinical trials to test existing drugs and rehabilitation methods for treating similar health disorders caused by chronic diseases of the heart and lung. Among the drugs to be tested are several kinds of cheap and widely available medicines in the world, such as aspirin and antihistamines.
The many findings expected to emerge from these studies will also be beneficial for understanding and treating other disorders that have the same or overlapping symptoms, like Lyme disease, chronic fatigue syndrome and complicated influenza (mostly found in the West). For the millions whose health has been weakened by the virus that has not yet ended, 2022 seems to be a year filled with hope.
In confronting all these, our health system and health care companies should prepare assistance for long Covid patients. Proper rehabilitation can prevent permanent damage to personal health and finances.
Business owners can employ people with disabilities while the government provides assistance through incentives. Besides, working from home and flexible rotating timetables will help long Covid patients remain active, at least on a part-time basis. Special clinics are needed for these patients to speed up their recovery, in the way hospital management was reformed when infections peaked so they could treat Covid-19 patients.

Syafiq Basri Assegaff
This was done to prevent people from having to shop around from one specialist to another to obtain accurate diagnosis. We should remember and continue to hope that many patients will recover, although this might take months. Many mistakes were made previously for during the phase of acute Covid-19 infection. There is no reason to fail again in responding to long Covid. There is no more time to waste.
Syafiq Basri Assegaff, Physician; alumnus of Padjadjaran University medical school; lecturer, Communication and Business Institute, London School of Public Relations, Jakarta
This article was translated by Aris Prawira