Optimism in Welcoming Vaccines
Almost all television stations broadcast live the arrival of a Garuda airplane at Soekarno-Hatta Airport carrying 1.2 million doses of the Covid-19 vaccine, a product of Sinovac, on 6 December 2020.

Even important state guests are not welcomed with such massive news coverage.
Almost all television stations broadcast live the arrival of a Garuda airplane at Soekarno-Hatta Airport carrying 1.2 million doses of the Covid-19 vaccine, a product of Sinovac, on 6 December 2020. The video of the plane unloading the large box of vaccine went viral.
The arrival of this vaccine truly got special treatment from the government. The vaccine is expected to be able to cope with the spike in (Covid-19) transmission, which until now has not decreased, even tends to rise sharply. Until the second week of December, the increase in the number of positive cases averaged over 5,000 cases per day, with an increase of about 150 deaths per day. The number of doctors and medical personnel who fell victim and died has exceeded 300 people. The situation is not improving and enforcement of health protocols is weak. Most of the activities that created crowds were not prosecuted.
In this situation, the arrival of the vaccine becomes a kind of oasis that promises freshness in the midst of a pandemic. Of course, (it will work effectively) if the vaccine has an emergency use authorization (EUA) permit from the Food and Drug Monitoring Agency (BPOM).
What arrived some time ago was a vaccine from Sinovac, China. The Health Minister has decided to use six Covid-19 vaccine candidates for the mass vaccination program, namely Bio Farma, Moderna, Astra-Zeneca, Pfizer-BioNTech and Sinovac-Biotech products.
Also read: Out of Faith, Serving as Volunteers
On the map of the vaccine race, this Sinovac product is not the favorite. The product has undergone clinical trials in Brazil, India, Turkey, Bangladesh and Indonesia. In Indonesia, this vaccine has not yet been completed. The third phase of the interim clinical trial report is scheduled for completion in January 2021. Last week, the head of communication for Bio Farma stated that the efficacy of the Sinovac vaccine reached 97 percent. This statement can mislead the public. As is known, the highest vaccine efficacy is currently held by the Pfizer vaccine with 95 percent.
This is the stage that determines the effectiveness and side effects of the vaccine being tested.
After several criticisms, then came an explanation by the spokesman of Sinovac, who stated that it was not efficacy, but seroconversion (the development of antibodies that can be detected on microorganisms in the serum). According to WHO, vaccine efficacy is the vaccine\'s ability to protect against disease in controlled clinical trials. The percentage of this vaccine\'s efficacy was obtained in Phase II clinical trials. This is the stage that determines the effectiveness and side effects of the vaccine being tested.
The Sinovac-Biotech product vaccine, which was tested in the third phase of the clinical trials in Brazil, showed less encouraging results. In early November, the Brazilian government suspended the process of a third clinical trial after a serious incident involving a volunteer. The Brazilian National Health Survey (ANVISA) did not specify what happened, but there are reports that indicate the incident could cause potentially fatal side effects, severe disability and other clinically significant.
Brazilian President Jair Bolsonaro had stated that his government would not buy the vaccine made by Sinovac. However, there was a follow-up report that said, after being traced, this incident was not because of the vaccine, but because the volunteer turned out to be in the group that was injected with a placebo or empty, there was no vaccine. This is a relief.

FILE - In this undated file photo issued by the University of Oxford on Monday, Nov. 23, 2020, a researcher in a laboratory at the Jenner Institute in Oxford, England, works on the coronavirus vaccine developed by AstraZeneca and Oxford University. With major COVID-19 vaccines showing high levels of protection, British officials are cautiously — and they stress cautiously — optimistic that life may start returning to normal by early April. Even before regulators have approved a single vaccine, the U.K. and countries across Europe are moving quickly to organize the distribution and delivery systems needed to inoculate millions of citizens.
In the map of the world vaccine race, the first place to finish is Pfizer-BioNTech\'s m-RNA-based BNT162B2 vaccine, which recently received emergency use approval from UK health authorities and the US Food and Drug Administration (FDA). Pfizer is headquartered in New York, founded in 1849, and BioNTech is a German biotech company founded in 2008 by the scientists Ughur Sahin and Ozlem Tureci.
Also read: Pope Urges Countries to Share Covid-19 Vaccines
The speed with which this approval was granted was due to its third phase clinical trial report published on 18 November, which concluded that the vaccine has 95 percent efficacy in volunteers who have not and have previously been infected with SARS-CoV-2. The UK has not even given approval to its domestic vaccine, the production of Astra-Zeneca in collaboration with Oxford. Quickly, Bahrain, Canada, Saudi Arabia, and Mexico followed suit with approval for the Pfizer-BioNTech vaccine.
Pfizer-BioNTech won the fast race to make the Covid-19 vaccine, but this vaccine is more troublesome. Apart from the matter of efficacy, safety and the ability to increase immunity, observers have criticized the Pfizer-BioNTech vaccine, which must be stored in a cooled room of minus 70 degrees Celsius. This will be inconvenient in the distribution and storage process, especially for developing countries that do not yet have refrigerated facilities of up to minus 80 degrees Celsius. The Astra-Zeneca vaccine is more flexible, can be transported and stored in a normal cooled room of minus 2-8 degrees Celsius, and is stable for up to six months. Moderna\'s m-RNA 1273 vaccine requires a refrigerated room of minus 20 degrees Celsius, and is stable for up to six months.
Responding to this criticism, Pfizer created its own supply chain and planned to distribute products directly to vaccination sites, using self-made coolers, and without the use of importers or agents. This way, Pfizer claims the vaccine can be stable for 10 days, and once it is removed from the container, it can last one day at a temperature of 2-8 degrees C. With this illustration, for Indonesia, it seems that the Pfizer-BioNTech vaccine is more troublesome compared to its competitors.
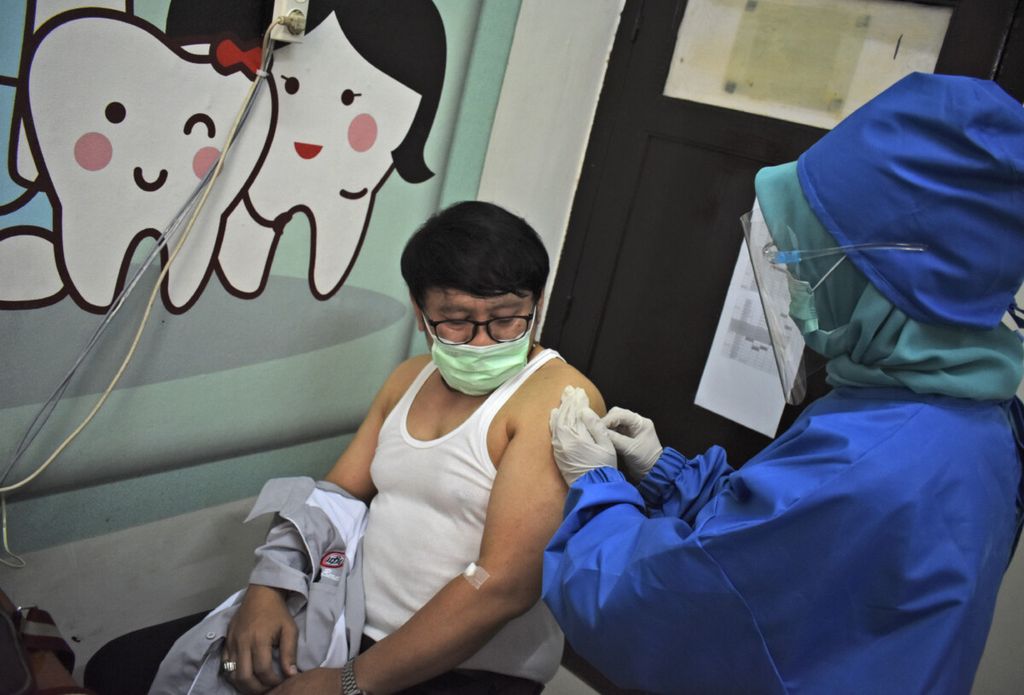
A medical worker gives coronavirus vaccine candidate to a volunteer during a trial at a community health center in Bandung, West Java, Indonesia, Friday, Aug. 14, 2020. Indonesia\'s only vaccine production company has started this week a so-called phase 3 clinical trials to test a potential coronavirus vaccine developed by a Chinese company. )
Regarding price, by far the cheapest vaccine was the one made by Astra-Zeneca. Reported by kompas.com (7/12/2020), the vaccine produced in
England in collaboration with Oxford costs around Rp 57,000 per dose. This vaccine is still in the process of being submitted for distribution authorization from UK health authorities. The Sinovac vaccine that has entered Indonesia is around Rp 200,000 (US$13.6), cheaper than those sold in China itself, around Rp 421,000 ($29.7).
The Johnson & Johnson vaccine is around Rp 141,000 ($10), Novavax is around Rp 226,000 ($16), Pfizer-Bio-NTech is around Rp 283,000 ($20) and the most expensive is the one produced by Moderna, Rp 350,000 to Rp 526,000 ($25-37) per dose.
MRNA and DNA methods
Pfizer-BioNTech’s BNT162b2 and Moderna’s mRNA-1273 vaccines need to be kept at cooler temperatures because they are both based on mRNA messenger ribonucleic acid (ribonucleic acid) technology. DNA (deoxyribonucleic acid) stores a set of genetic instructions that play a role in the growth and development of every living cell, including viruses. Well, this m-RNA uses a fat membrane to send instructions stored in the core. In this case, it’s the instructions to increase protein production in the SARS-CoV-2 spike virus in human cells (duplicating SARS-CoV-2, only the legs that appears in human cells).
Also read: Vaccines and Economic Recovery
This is a way to train the body\'s immune system. Upon seeing the "appearance" of SARS-CoV-2\'s legs, human immune cells were immediately provoked and reacted quickly sending troops to muzzle the cells and “memorize” the legs. In fact, what it was fighting was the appearance of the "legs" of the virus, not the real virus. Because they have been trained, if one day they are infected with a real virus, the body\'s immune system already knows its job: immediately suppresses it. This is a simple description of the mechanism of action of vaccines based on the mRNA method.
Then the body will respond by producing antibodies or immunity.
Meanwhile, Astra-Zeneca uses the classic DNA method, which uses an adenovirus (DNA virus) which has been attenuated and can be inserted with other genetic materials. Astra-Zeneca uses the common cold virus whose genetic makeup has changed so that it cannot live actively in the human body. This inactivated virus is then inserted with pathogenic (disease-causing) genetic material, namely protein spikes, and then inserted into the nucleus of the vaccinated person. Once infected, it produces an increase in protein spikes, which the early warning system will detect as an attack. Then the body will respond by producing antibodies or immunity.
So, the difference is, the m-RNA vaccine uses a fat membrane to send instructions to produce a protein spike, while the DNA vaccine uses an adenovirus to be infected into cells. Each of these methods has drawbacks. DNA vaccines can integrate/bind with human cell DNA which can potentially mess with human genes/mutations. Although the long-term effects of this integration have not been observed, it is not a good thing for the human body.
Besides, adenovirus is a virus that is commonly found in everyday life and has most likely infected the body of someone who is going to be vaccinated. This allows the adenovirus vaccine to be destroyed by the human body before it enters human cells and creates immunity. On the other hand, the m-RNA vaccine can potentially trigger inflammation that DNA vaccines do not experience.

Sao Paulo Governor Joao Doria poses for photos holding a dose of the CoronaVac vaccine against COVID-19 next to a container unloaded from a cargo plane that arrived from China at Guarulhos International Airport in Guarulhos, Sao Paulo state, Brazil, on December 18, 2020. - Brazil received Friday the third lot with 1,900,000 doses of the CoronaVac vaccine, developed by the Chinese laboratory Sinovac Biotech.
There are a few notes. The Sinovac vaccine is clinically tested in Indonesia on people aged 18-59 years old. This means that for people 60 years old and over, it is not possible to know the efficacy, safety and immune effects. On the other hand, the Pfizer-BioNTech vaccine has been used for the first vaccination in the UK, last 8 December and the recipient was Margaret Keenan, a 90-year-old woman. This means that people aged 60 years and over who are not sure about the Sinovac vaccine can use the Pfizer-BioNTech vaccine.
Of course the vaccine is not only Sinovac so that the budget could be bigger.
Vaccine’s big money Coordinating Human Development and Culture Minister Muhadjir Effendy said the government will provide vaccines for 182 million people, an increase from the original target of 107 million (67 percent of the population aged 18-59 years old). Seeing the age range of 18-59 years old, surely it refers to the Sinovac vaccine. If you refer to Bio Farma\'s statement that the price of Sinovac vaccine is around Rp 200,000, and each person needs to be vaccinated twice, there will be a circulation of at least Rp 72 trillion. If the government purchases this for free vaccination, that means money from the state budget. Of course the vaccine is not only Sinovac so that the budget could be bigger. It\'s a giant business. Vaccine importers can get huge profits from the sale of this vaccine.
Also read: Voices of Strong Women amid Pandemic
Behind big money can be a danger. We have just learned a lesson. In the mid of a pandemic there are still hands that can commit corruption. The Social Affairs Minister and his subordinates were arrested by the KPK on suspicion of misuse of social assistance funds distributed to citizens affected by the pandemic. We hope that this vaccination plan can run smoothly, without abuse of power and finances.
Vaccination is an expectation based on scientific principles. Of the total vaccine candidates, prioritize the vaccine that best meets the criteria for Indonesia\'s conditions. The decision of the government to cooperate with the five most potential vaccine candidates was correct. This means that the vaccination plan does not depend on only one vaccine product. As long as the efficacy, safety and ability to generate immunity meet the medical standards and the price is affordable, vaccination can be a foundation to contain the pace of the pandemic so that the curve can flatten and then decline.
Keep in mind, the curve of the number of Covid-19 cases is inversely related to the economic growth curve. If the curve of positive cases flattens and decreases, the risk of transmission will be smaller so that the Health Ministry and the Covid-19 task force can loosen up economic and social activities again. This way, the economic growth curve will gradually increase.

Djoko Santoso
The success of vaccination will raise our enthusiasm and optimism. Before the vaccine is injected, it is necessary for the government to improve its communications. Be honest about the benefits and the risks. If the vaccine is claimed to be safe, give an example by being the first to be vaccinated. Actions are more convincing than any beautiful words to convince the people.
DJOKO SANTOSO, Professor of Medical Sciences Unair