Anticipating Covid-19 Vaccine
Covid-19 transmission across the world is still increasing. The number of cases accounts for 36 million people and about a million people have died.
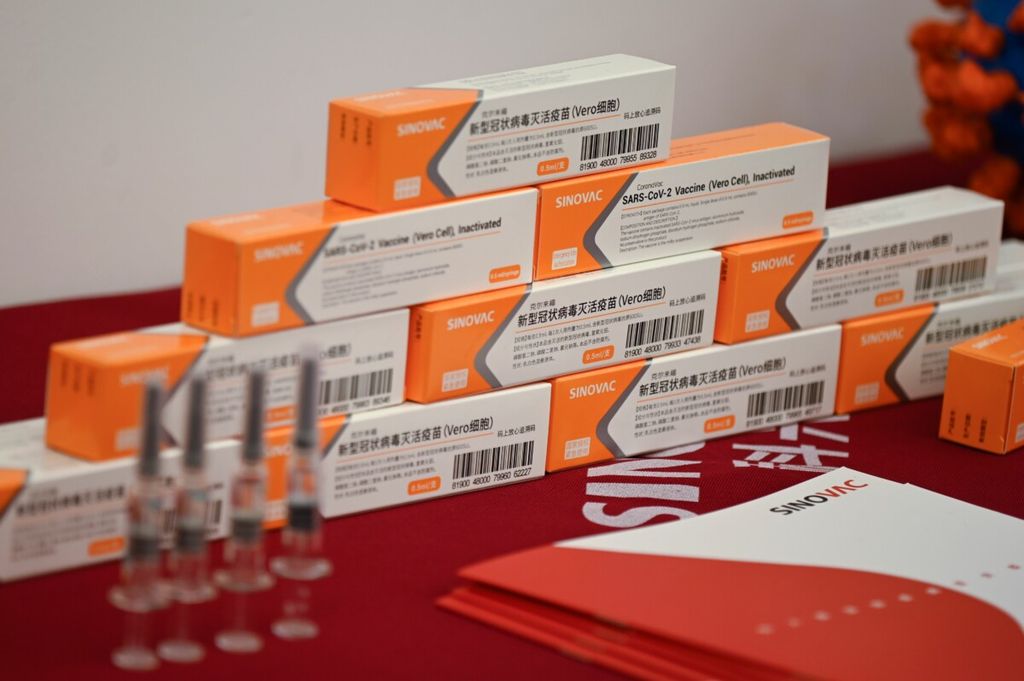
Sinovac Biotech vaccines, one of 11 Chinese companies approved to carry out clinical trials of potential coronavirus vaccines, are displayed at a press conference during a media tour of a new factory built to produce Covid-19 coronavirus vaccines, in Beijing on September 24, 2020.
Covid-19 transmission across the world is still increasing. The number of cases accounts for 36 million people and about a million people have died. In Indonesia, as of 7 October 2020, more than 311,000 people had been infected, more than 11,000 people had died and the number of cases has increased by 3,000-4,000 people per day.
Today, countries across the world apply health protocols as the main measure to put a brake on pandemic expansion, especially because there is no medicine that is really effective and vaccines are still much-awaited. For medicine, many studies have been conducted, and the World Health Organization (WHO) has even carried out a Solidarity Trial involving dozens of countries (including Indonesia) to then issue recommendations on drugs for this disease.
Also read: The Race to Creating a Vaccine
Now, there are discussions about the Solidarity Trial for vaccines with their various implications and complexities.
Decades
Vaccines are indeed humanity\'s great hope as one of the main weapons to control Covid-19. Thus, various institutions are competing to conduct research to create ones. Of course, we all hope that the results will be good. But, we need to be aware of the existing facts.
So far, it takes dozens of years for researchers to find the vaccines from the first time the virus was found. The new polio vaccine was discovered in 1954 or 45 years after the virus was discovered in 1909. The measles vaccine was only discovered 46 years after the disease was found and the hepatitis B vaccine was found only 17 years after the virus was discovered. Covid-19 was discovered in December 2019 and by this time it is now just 10 months. (So, it seems we still have to wait).
Also read : One More Step to Take for Vaccine
Of course, the development of science has progressed very rapidly, so it is possible that the decades in the past era could now have been shortened to around one year. However, because this vaccine will be given to all mankind, no matter how sophisticated the technique, there must be a guarantee that the vaccine is truly safe for humans, and, of course it must be effective in preventing disease transmission.

An engineer works in the general laboratory during a media tour of a new factory built to produce a COVID-19 coronavirus vaccine at Sinovac, one of 11 Chinese companies approved to carry out clinical trials of potential coronavirus vaccines, in Beijing on September 24, 2020.
Vaccine production can come from various sources or mechanisms. There are vaccines that are made from viruses that are attenuated or inactivated, some are from DNA or RNA, some are called replicating and some are non-replicating viral vectors, and there are also protein sub-units and viruses like particles. Each vaccine candidate can use one of these mechanisms, and the results will also likely have its own specifications.
Also read : Key to being at Peace with Coronavirus
Data from WHO\'s COVID-Vaccine Landscape on 25 September 2020, shows that there are already 40 vaccine candidates that have entered clinical trials, nine of which are already in Phase III (one of which is currently being tested in Bandung) and 149 are still at the preclinical stage, meaning that they are still at the laboratory and not yet tested on humans. Phase III clinical trials are very advanced in stage and, if successful, will be ready for mass production. Of course, we all realize that undergoing "tests" in any form, some may pass and some may not. Among those who passed the test, there were those with good scores and some who were not. In the case of Phase III clinical trials, some vaccines in the past (for past diseases) have worked, some have failed.
Anticipation
If the vaccine that is currently being clinically tested has succeeded in preventing people from contracting Covid-19 – as we have expected -- there are at least five things that need attention and we anticipate from now on so that the Indonesian people are ready to face the various possible realities that exist. First, is the protective capability really 100 percent, or maybe less, maybe 70 percent or even 50 percent? If someone is already vaccinated, is there still a chance that he or she still have the possibility of being infected?
A research in the United States shows to eliminate a pandemic (if we only rely on vaccines alone without social distancing), we need to vaccinate 100 percent or the whole population (something very, very difficult) if the effectiveness of the vaccine is only 60 percent; and if we can only vaccinate 75 percent of the population, the effectiveness of the vaccine must be at least 80 percent.
Also read : Waiting for COVID-19 Vaccine
Second, how long the protective capacity (of the vaccine) will last? Data on how long the immunity lasts among recovered patients so far is still limited and some studies say it only lasts for months. Third, is the administering of the vaccine, whether only once or twice at the beginning. Then, does it need to be repeated after the next few months/years, or does it need a booster and so on.
This will greatly affect policy management, including the financial aspect, because if the vaccine administering has to be repeated (to everyone), the budget prepared must be several rupiah (or US dollar), multiplied with a few hundred million people. That is not a small amount.
Fourth, whether the distribution (of the vaccine) in the field is relatively easy or maybe it needs certain conditions (maybe it needs to be stored in a low temperature so that it is not damaged, etc.). This will depend on the type of vaccine, and of course have an important impact, especially in remote areas with difficult transportation in our country. This distribution will involve millions of people, including health workers, transportation, management, security, community participation mobilization and others.
Also read: Infodemic on Medicines for COVID-19
Fifth, whether the new vaccine be administered on everyone, including the elderly, pregnant women or children? Some vaccine trials are now only conducted in certain age groups, for example, the clinical trials involved people no older than 59 years old. So, we do not know how the impact will be on elder people. Also, (the trials) do not include certain community groups (pregnant women, groups with hold low body, etc.). In fact, in the future everyone will have to get the vaccine, so it is necessary to think about a solution.
All these questions can only be answered when Phase III clinical trials have been completed, both those currently being conducted in Bandung and those currently being carried out simultaneously in a number of other countries. The final result will be compiled and analyzed in depth. In fact, there are also many questions about the sixth point, namely whether virus mutations that have occurred (including in Indonesia), as well as certain antibodies, will affect the effectiveness of the vaccines that are being manufactured. The data so far still prove that various vaccine candidates are likely to be able to deal with changes due to the current mutation.
Vaccines for all
After the vaccine really exists, there must be assurance that everyone will get it, “vaccine for all” so that (virus) transmission on earth can be stopped. This is also in line with the principle of "no one is save until everyone is save". If there is still a source of transmission, of course it will still be possible for other people to be infected and the pandemic cycle that has destroyed various aspects of life will continue.
In this case, WHO and various international agencies have established a CO-VAX facility which will support countries across the world in procuring the Covid-19 vaccine when it becomes available. The capabilities of countries vary, of course. On the other hand, in the early days of mass production, the number (of vaccine) would certainly not be sufficient for all global population. Therefore, distribution will be made in stages, which WHO calls the “allocation framework”.
Also read : Clinical Trials to Finish in Early 2021
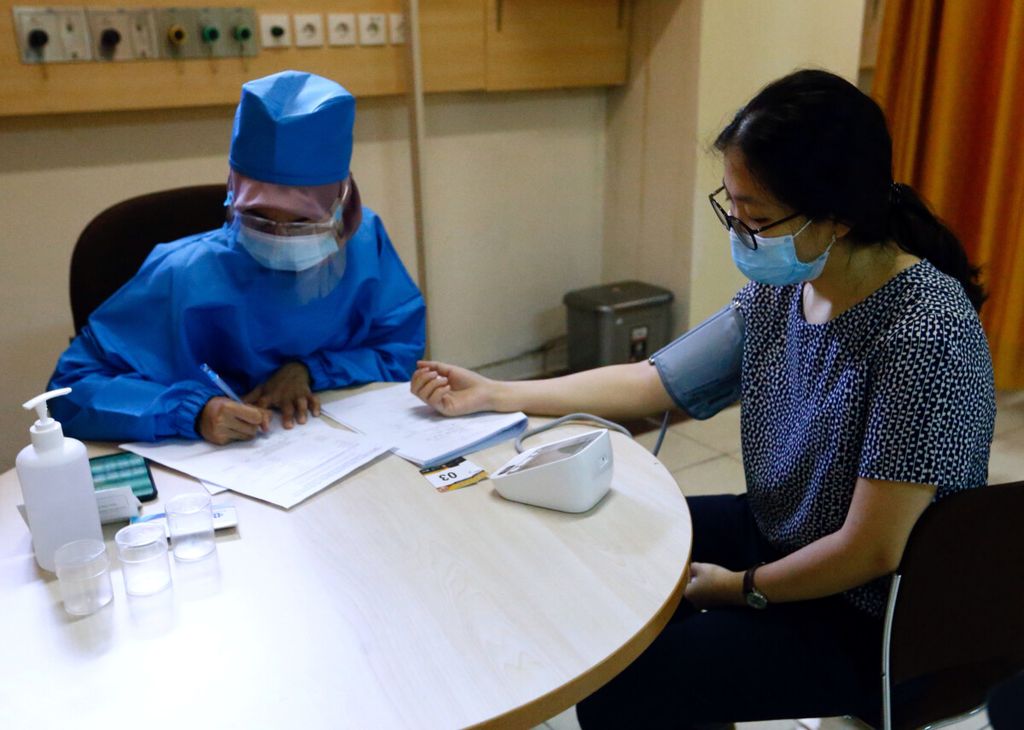
A healthcare worker checks the tension of a volunteer during a simulation for coronavirus vaccine clinical trials next week at the Faculty of Medicine at Padjadjaran University amid the COVID-19 pandemic in Bandung, Indonesia, August 6, 2020.
So far, the recommendation is that at the beginning there will be at least 3 percent of the vaccines that will be allocated to health workers and other field social workers. Then, about 20 percent of vaccines will be prioritized for high-risk groups, including the elderly, those with comorbidities (co-morbid) and others based on special considerations. If then the supply has increased, of course it will cover the entire community at large.
It must be remembered that vaccinating all people in a country is certainly not a simple matter. Perhaps, many countries have long experience giving vaccines to all children. However, if it is for all people of all age groups, distribution management will be very complex, involving political policies at all levels, human resources, work systems, socio-cultural aspects, mass mobilization, community participation, demographics, finance and etc.
Also read : Like Atomic Bomb, Covid-19 Vaccine Will End ‘War’
Not to mention the case that there may (and seems to always be) individuals who refuse to be vaccinated for various reasons. In addition, it is possible for a country to use several types/brands of vaccines at once, with various variations. It must also be noted that there will be post-marketing surveillance activities, namely observing the results of vaccines that have been used in the field, whether everything is good (according to the results of clinical trials) or are there other unexpected effects. All of this needs to be prepared in great detail from now on, with only three months left before the start of 2021, including the contingency plans, given the possible challenges in the field.
President Jokowi\'s directive clearly states that a detailed plan for the delivery of the Covid-19 vaccine needs to be drawn up and this should be available in the near future.

Tjandra Yoga Aditama
While we are waiting for the development of vaccines (and also drugs) for Covid-19 (it seems that even after the vaccines exist, they are not yet effective enough to cover all populations), indeed we must rely fully on health protocols, from the basic to perhaps strict social restrictions. For this, the right policies, firm regulations, massive outreach, monitoring and evaluation of pandemic situations based on scientific evidence, and the active participation of all parties are of utmost importance.
The Covid-19 pandemic, which has completely ravaged the world has again proven that "Health is not everything, but without health everything is nothing".
Tjandra Yoga Aditama, Professor in Pulmonology, University of Indonesia; former director of WHO SEARO and former director general of disease prevention and control (P2P) and head of health research and development at the Health Ministry.